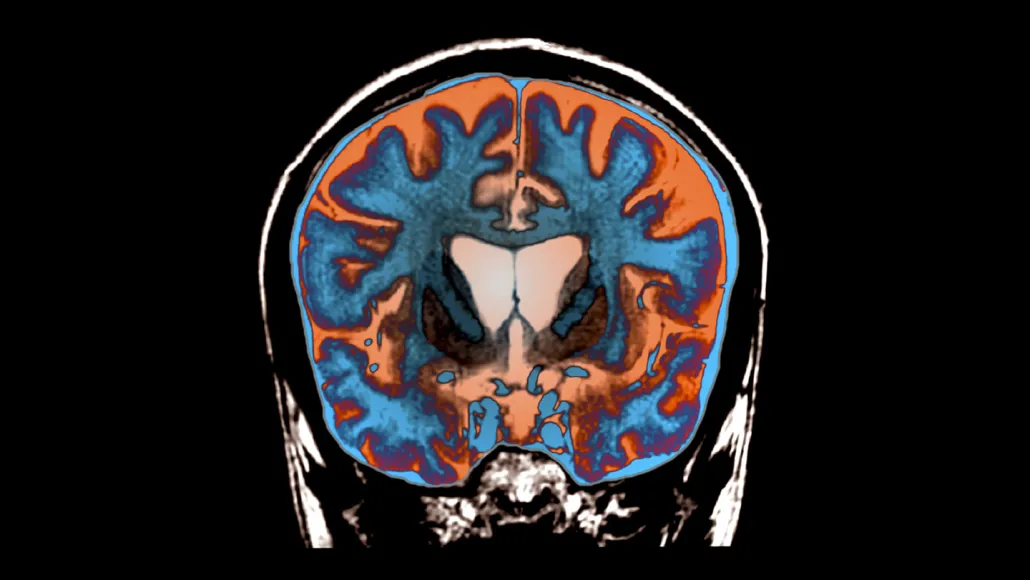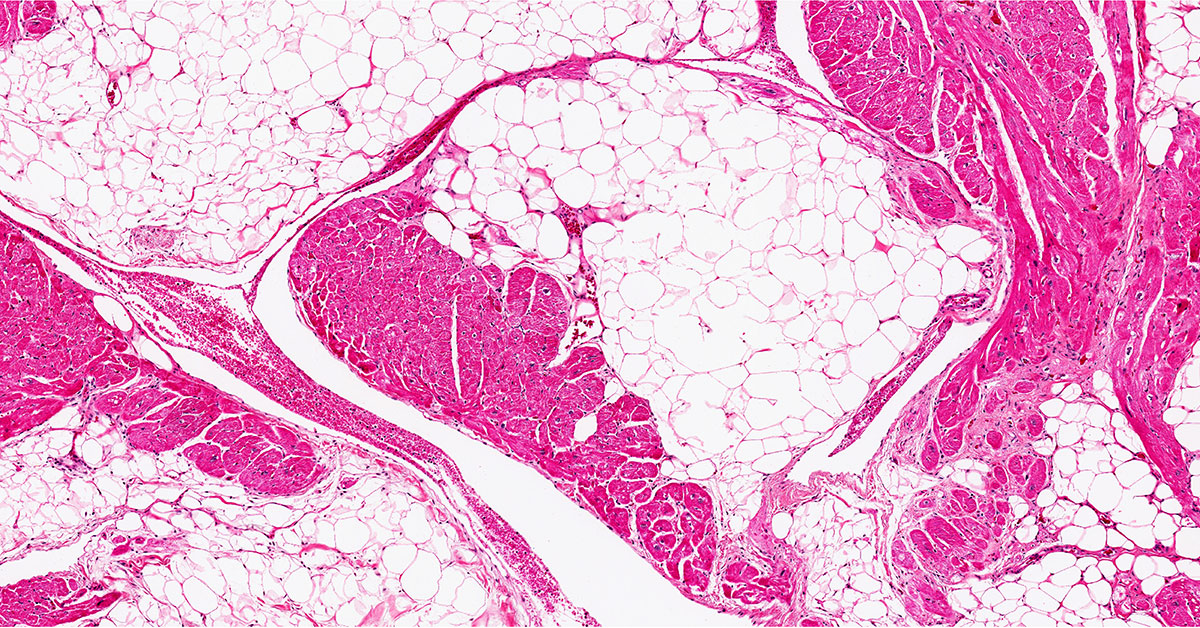
Cardiac fibrosis is the slow scarring of heart tissue that follows heart attacks, chronic hypertension, and a range of other heart conditions. Once it sets in, it stiffens the heart, impairs its ability to pump, and contributes substantially to the eventual progression to heart failure. Despite how central it is to cardiovascular mortality, there are no approved therapies that reverse or even reliably slow it.
A line of research presented in 2025, led in part by groups at Penn and Northwestern, takes an approach that combines two technologies that have already proved transformative in other fields: CAR-T cell therapy from cancer immunology, and mRNA delivery from the COVID vaccine era. The strategy targets activated fibroblasts — the cells that lay down scar tissue — and instructs the immune system to clear them.
In conventional CAR-T therapy, a patient's T cells are removed, genetically engineered to express a chimeric antigen receptor that recognizes a target on diseased cells, and reinfused. The cells then hunt and destroy their target. For cardiac fibrosis, the approach is similar in concept but different in execution: rather than engineering cells outside the body, researchers use mRNA delivered by lipid nanoparticles to instruct the patient's own T cells in place. The mRNA encodes a CAR specific to a marker found on activated cardiac fibroblasts. T cells take up the instructions, briefly express the receptor, attack the fibroblasts, and then return to baseline as the mRNA degrades.
In mouse models, the approach has reduced fibrosis and improved cardiac function after experimentally induced injury. The transient nature of the mRNA-delivered CAR is appealing as a safety mechanism — the treatment effectively turns itself off — and it sidesteps the elaborate cell-engineering pipeline that makes conventional CAR-T expensive and slow to administer.
Translating the strategy into people will require resolving several open questions: whether the same fibroblast marker is reliably present and specific in human hearts, how to dose the therapy in a chronic condition, and how to ensure the treated fibroblasts don't simply return as the underlying drivers of fibrosis persist. Early-phase human trials are being designed.